Stran trenutno ni na voljo v vašem jeziku. Lahko si ogledate strojni prevod, ustvarjen s storitvijo Google Translate. Te storitve ne zagotavljamo mi in rezultatov prevoda nismo preverili.
Za dodatno pomoč se lahko obrnete na nas.
Adding to survival chances - pioneering brain disease treatment relies on 3D printing
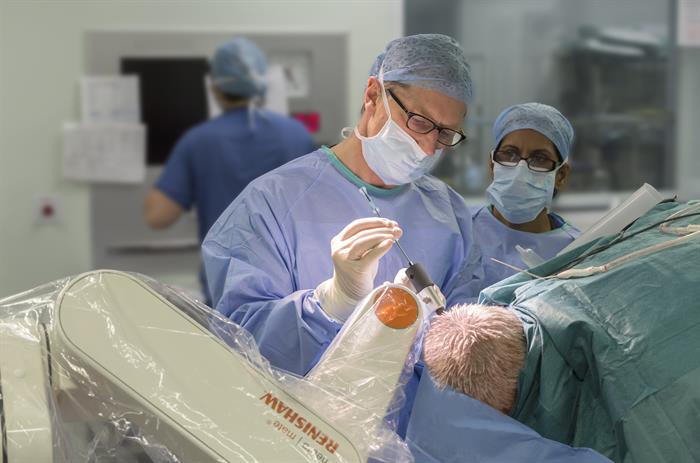
Diffuse intrinsic pontine glioma (DIPG) is a rare but deadly brain tumour. No child has ever survived it, most becoming paralysed and dying in just a few months. Now an novel investigational drug delivery system, which delivers therapeutic agents directly to tumours deep within the brain, is being used by a team in Bristol. This therapy uses a sophisticated drug delivery system that relies on additive manufacturing (AM) to produce critical components.
And cancer is just one of many possible applications for this technology. Other debilitating and ultimately deadly conditions such as Parkinson's Disease are also being treated this way in clinical trials.
I'll explain how AM is involved in this pioneering therapy a little later. First some context...
Circumventing the blood-brain barrier
Treating cancers and other abnormalities in the brain is particularly difficult. For instance, chemotherapy normally relies on our body's blood stream to deliver the cytotoxic drugs to the tumour site to kill the cancer cells. This works well elsewhere in the body where the drugs diffuse from the blood into the cancer tissue, but our brain is different. It is protected by the 'blood-brain barrier' (BBB), comprised of endothelial cells, which separates our blood from the extra-cellular fluid in our central nervous system.
This barrier is selectively permeable, only letting through those substances that will not damage our brain. Most diagnostic and therapeutic agents are repelled. Disruption of the BBB is possible, but the efficacy of this technique has been questioned (ICSI, 2001; CMS, 2007) and it is associated with a higher risk of complications than conventional chemotherapy.
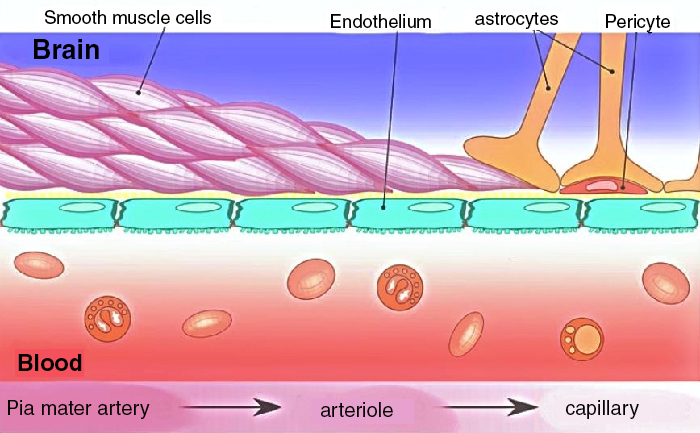
Image above from Wikipedia
Testing new therapies
So neurosurgeons are developing ways to deliver chemotherapy directly into the cancer tumour, bypassing the BBB. One pioneer of this intra-parenchymal drug delivery technique is Professor Steven Gill at the Bristol Royal Hospital for Children. This Mail Online article describes Prof. Gill's work and the fund-raising initiatives to pay for full clinical trials.
In the case of Parkinson's Disease, a clinician-led phase II trial at North Bristol NHS Trust has been running since 2013 using a drug called Glial Cell Line-Derived Neurotrophic Factor (GDNF). The results of this phase II study are expected later in 2016.
The modern neurosurgeon's toolkit
Delivering drugs to target anatomy located deep within the brain requires planning, precision and some sophisticated medical devices. Renishaw supports neurosurgeons with a range of technologies that are designed to accurately deliver implantable devices with the aim of improving patient outcomes.
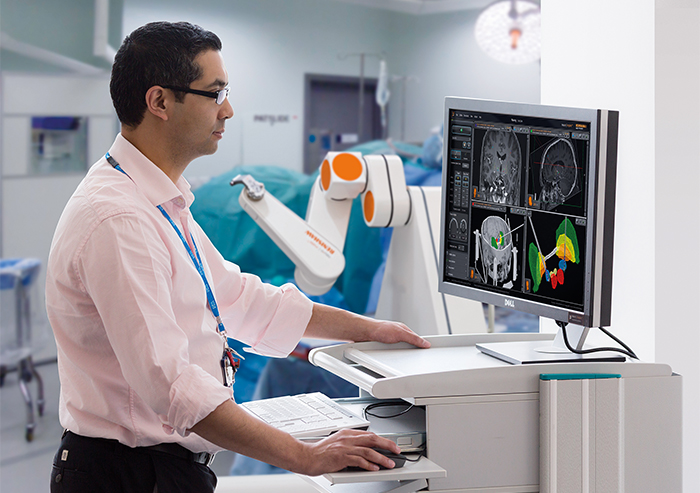
Image above: Surgical planning software and stereotactic robot at Bristol Royal Hospital.
Renishaw's neuroinspire™ surgical planning software (shown below) helps neurosurgeons to plan their surgical procedure.
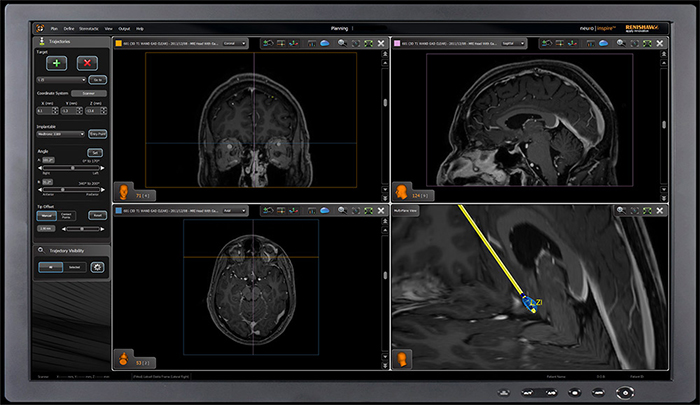
The neuromate® stereotactic robot (shown below) provides consistent, rapid and precise targeting during neurosurgical procedures.
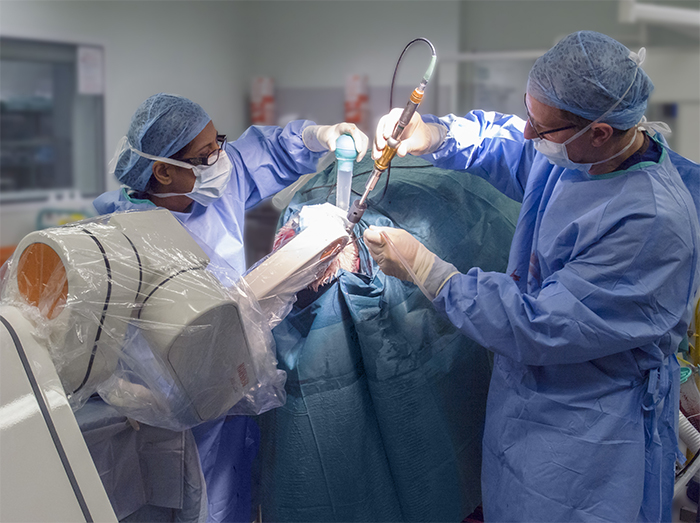
Using these techniques, one or more implantable devices can be inserted at defined angles through small holes drilled in the patient's cranium, precisely targeting anatomy deep within the brain. These implants can be electrodes to stimulate or sense activity inside the brain, or micro-catheters to deliver therapeutic agents directly into brain tissue.
Convection-enhanced drug delivery
Intra-parenchymal drug delivery offers a practical method of bypassing the blood-brain barrier and shows great promise in providing the next step change in the treatment of neurodegenerative, neuro oncology and other debilitating neurological conditions.
Over the last 3 decades there has been an increasing number of authors reporting on its potential through novel delivery methods such as Convection Enhanced Delivery (CED).
The new brain cancer therapy involves a drug delivery system featuring multiple micro-catheters. Using CED, a pressure gradient is established at the tip of a catheter to infuse a therapeutic agent.
The intention is to distribute the drug more evenly, at higher concentrations, and over a larger area than when administered by diffusion alone. Another advantage of CED is that the blood brain barrier acts to keep the drug within the brain tissue where it is needed, so minimising unwanted side-effects.
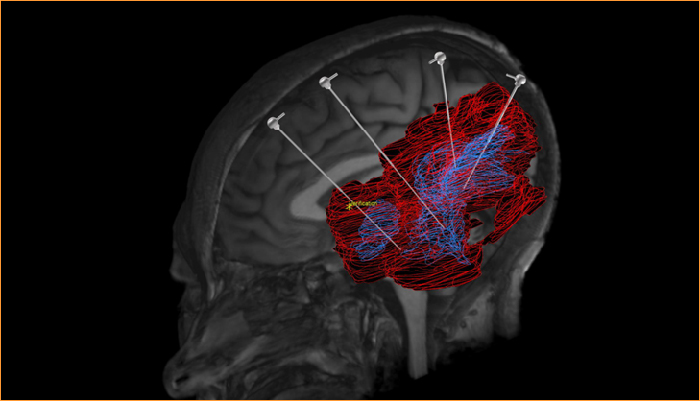
Image above: proposed intra-parenchymal drug delivery clinical trial set-up
The drug delivery system is shown below. In this diagram, four micro-catheters have been placed through burr holes in the patient's skull. Each is fed by a small tube through which the therapeutic drug is transmitted. These tubes come together in a manifold on the top of the skull, and the feeder tube is passed under the patient's skin to a bone-anchored transcutaneous port behind the ear.
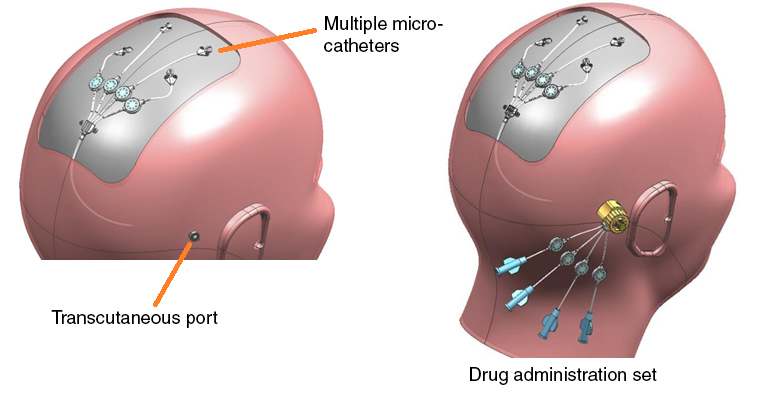
The drug administration set can then be attached to this port to feed drugs into the patient's brain. This can be done intermittently using infusion pumps to control the rate at which the drug is delivered.
So what's all this got to do with AM?
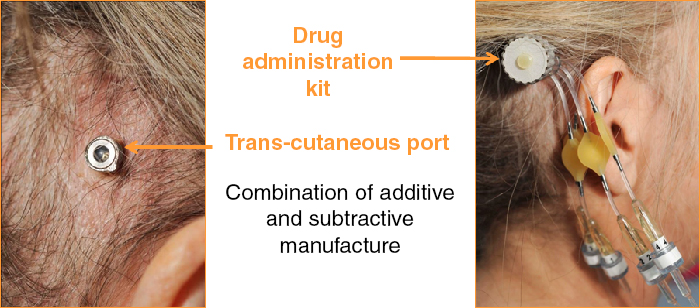
The bone-anchored transcutaneous port and the connecting manifold on the drug administration kit form a critical connection point. They provide a secure and hygienic connection through which drugs can be infused simultaneously in each of four catheters.
The transcutaneous port is bone-mounted and so includes features such as external ribs and a textured surface to make it bio-integratable - features for which AM is an ideal manufacturing process. The port also contains small, intricate internal channels through which drugs can pass into a subcutaneous tube, and a sealed septum to prevent infection. These holes and the flat septum surface require levels of precision beyond those that can be achieved with AM, so the parts are produced with a 'hybrid' process including both AM and machining.

It's a similar story for the administration manifold, which also includes internal micro-channels and a 'living hinge' that is used to snap it into place on the transcutaneous port. Small side-venting needles are pressed into the manifold to deliver the drugs into the port in a way that prevents debris from being pushed into the micro-channels attached to the patient. Once again, a hybrid manufacturing process is employed.
Summary
The engineering challenges to successfully deliver these pioneering therapies are intense. It is by combining metrology, robotics, additive manufacturing and precision machining, that we can meet these challenges and bring hope to families faced with a brain cancers, neurodegenerative and 'orphan' diseases.
Next Steps
To find out more about the capabilities of AM and the impact that it could have on your products and business model, check out my posts Additive impact part #1 and Additive impact part #2.
If you would like to explore how AM could be applied to improve your product in one of our AM Solutions Centres, then check out Making metal AM more accessible.